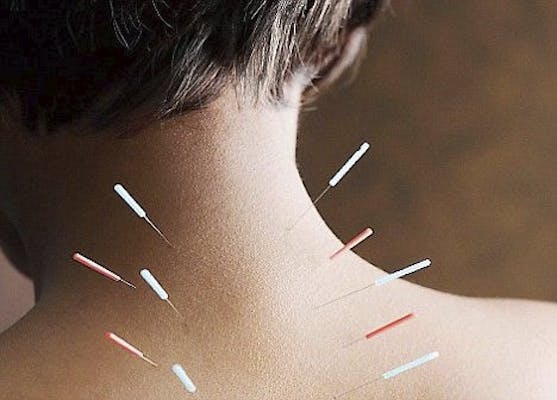
What is Dry Needling
Dry needling involves thin filiform needles that penetrate the skin and underlying muscle and connective tissues. The technique uses a "dry" needle without injection of medication inserted through the skin into areas of the muscle. It allows access to target tissues that may not be accessible with manual palpation. Dry needling is used to treat myofascial pain and trigger points but can also be beneficial for other musculoskeletal conditions such as neck and back pain, hip, knee and shoulder osteoarthritis, plantar fasciitis, temporomandibular joint issues (TMJ/TMD), nerve pain such as "sciatica" or carpal tunnel syndrome, rotator cuff issues, lateral epicondylitis, and Achilles tendinitis to name a few. The American Physical Therapy Association defines dry needling as a technique used to treat dysfunction of skeletal muscle and connective tissue, minimize peripheral nociception (pain), and improve or regulate structural or functional damage.
What is a Trigger Point
Trigger points are localized, hyperirritable spots located in a taut band of skeletal muscle. They produce pain and often accompany chronic musculoskeletal disorders. Injury, stress, poor posture or repetitive microtrauma may lead to the development of trigger points. Trigger points can be tender to the touch and palpation of a trigger point may cause or "trigger" pain to other parts of the body and when pressure is applied may elicit a local twitch response or "jump response" from the patient.
The Pain, Inflammation, Trigger point, Sensitization cycle
Following an injury, chronic pain, improper ergonomics, posture or static positioning, excessive acetylcholine (Ach) and subsequent calcium release can initiate a continuous cycle of localized intrafusal (muscle spindle) activation. This low-grade muscle contraction begins to deplete tissue oxygen and leads to local ischemia and hypoxia with subsequent release of a number of chemicals such as prostaglandins, serotonin, bradykinin and substance P, which causes local tissue sensitivity and pain. It also stimulates alpha and motor neurons which lead to further muscle tension and sensitivity of muscle spindles. This whole cascade causes a steady cycle of continued local tissue pain, inflammation, sensitivity and muscle tightness with myofascial trigger points.
Effects of Dry Needling
Dry needling releases or in-activates trigger points which decreases pain, muscle guarding and restores range of motion. Preliminary research supports that dry needling improves pain control, reduces muscle tension, and normalizes dysfunctions of the motor end plates, the sites at which nerve impulses are transmitted to muscles. This can help speed up the patient's return to active rehabilitation. Although still being researched, dry needling has been shown to reduce pain, decrease tissue sensitivity and release myofascial trigger points by several mechanisms some of which include:
- Stimulates release of ATP and histamine which reduces pain
- Stimulates fibroblasts which promotes collagen repair
- Releases myofascial trigger points by inhibiting alpha & gamma motor neurons
- Inhibits pain through both central and peripheral nervous system
- Inhibits inflammatory cytokines and substance P
- Stimulates the bodies' natural endogenous opioids such as GABA, endorphins & enkephalins for pain reduction
- Increases local blood flow to tissues via vasodilation
- Reduced "central sensitization"
- Break up or release scar tissue
Dry Needling at OSPT
Dr. Teixeira (Cert. DN) received his certification in Dry Needling 1 and 2 from the American Academy of Manipulative Therapy in 2017. He has used the technique daily with his patients and has been very impressed with the results. Dr. Teixeira uses the "in situ" method of inserting, then slightly turning needles, to wind and activate collagen fibers and then leaving them in for approximately 7-10 minutes which has been shown to be more effective than the simple in/out "pistoning" method of dry needling.
Reference: Peripheral and Spinal Mechanisms of Pain and Dry Needling Mediated Analgesia: A Clinical Resource Guide for Health Care Professionals Int J Phys Med Rehab 2016 4:2
